Overview
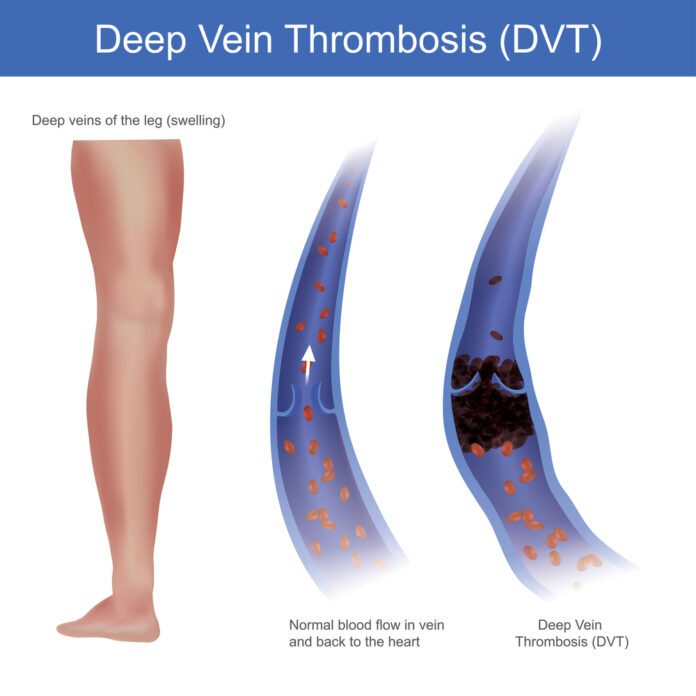
Deep vein thrombosis (DVT) is a blood clot that develops within a deep vein in the body, usually in the leg.
Blood clots that develop in a vein are also known as venous thrombosis.
DVT usually occurs in a deep leg vein, a larger vein that runs through the muscles of the calf and the thigh. It can also occur in the pelvis or abdomen.
It can cause pain and swelling in the leg and may lead to complications such as pulmonary embolism. Pulmonary embolism is the sudden blockage of a major blood vessel (artery) in the lung, usually by a blood clot. In most cases, the clots are small and are not deadly, but they can damage the lung. But if the clot is large and stops blood flow to the lung, it can be deadly.
DVT and pulmonary embolism together are known as venous thromboembolism (VTE).
Cause
DVT is caused by a blood clot. The clot blocks a vein, preventing blood from properly circulating in the body. Clotting may occur for several reasons.
These include:
● Injury. Damage to a blood vessel’s wall can narrow or block blood flow. A blood clot may form as a result.
● Surgery. Blood vessels can be damaged during surgery, which can lead to the development of a blood clot. Bed rest with little to no movement after surgery may also increase the risk of developing a blood clot.
● Reduced mobility or inactivity. When sitting frequently, blood can collect in the legs, especially the lower parts. If unable to move for extended periods, the blood flow in the legs can slow down. This can cause a clot to develop.
● Certain medications. Some medications increase the chances the blood will form a clot.
Symptoms
DVT symptoms: In some cases, there may be no symptoms of DVT.
If symptoms do occur they can include:
● pain, swelling, and tenderness in one of the legs (usually calf or thigh)
● a heavy ache in the affected area
● warm skin in the area of the clot
● red skin, particularly at the back of the leg below the knee
DVT usually (although not always) affects one leg. The pain may be worse when you bend the foot upward towards the knee.
Treatment
DVT treatments focus on keeping the clot from growing. Also, treatment may help prevent a pulmonary embolism and lower the risk of having more clots.
There are many ways to treat DVT. The most common forms of treatment include blood thinners and Catheter-Directed Thrombolysis. If the DVT has caused surface veins, there are vein treatment options such as Injection Sclerotherapy, a procedure in which a fine needle is used to shrink the veins.
Blood Thinners
These drugs, also called anticoagulants, are the most common treatment for DVT. They can keep a clot from growing or breaking off, and they prevent new clots from forming. But they can’t thin the blood, despite their name, or dissolve an existing clot.
Catheter-Directed Thrombolysis
Catheter-directed thrombolysis is a minimally invasive treatment that dissolves abnormal blood clots in blood vessels to help improve blood flow and prevent damage to tissues and organs.
When blood does not flow smoothly through a vessel, it can begin to coagulate, turning from a free-flowing liquid to a semi-solid gel, or blood clots. A blood clot, or thrombus, that forms within a blood vessel may continue to grow, blocking off the blood supply to certain parts of the body and causing damage to tissues and organs. In some patients, blood clots come from one site, dislodge, travel downstream, and lodge in relatively small vessels causing a blockage, or embolization. Untreated, a vascular blockage due to thrombosis or embolization can result in the loss of an organ or extremity, with potentially life-threatening consequences.
In a catheter-directed thrombolysis procedure, x-ray imaging is used to help guide a special medication or medical device to the site of blood clots to dissolve the blockage.
Other
Effects
One common complication of DVT is known as post-thrombotic syndrome. People with this syndrome may have a swollen leg that feels heavy and hurts. The skin on their leg may also become discolored and itch, and a rash may develop. More severe cases of post-thrombotic syndrome can lead to the formation of chronic wounds.
Post-thrombotic syndrome occurs if the DVT has damaged the walls or valves of a vein, causing the blood to constantly build up in the vein. The syndrome often only develops several weeks or months after the DVT, sometimes even after one or two years.
Pulmonary embolism
A rarer but more serious complication of deep vein thrombosis is known as pulmonary embolism. This happens if the blood clot breaks away from its original site and is carried in the blood to the lungs, where it blocks a blood vessel.
The symptoms of pulmonary embolism include:
• Sudden shortness of breath
• Chest pain (particularly when breathing in or coughing)
• Dizziness, lightheadedness, or unconsciousness
• Rapid heartbeat
• Coughing up blood (rare)
Pulmonary embolism needs to be treated quickly because the blocked blood vessel causes blood to build up between the heart and lungs. This can put too much strain on the heart and eventually lead to life-threatening heart failure.
If pulmonary embolism develops, then it usually does so within two weeks of the DVT. The risk of pulmonary embolism is greater if the thrombosis is in the upper part of your leg or in your pelvis than if you have DVT in your lower leg. This is also true for thrombosis that causes very noticeable symptoms.
Source
https://www.nhsinform.scot/illnesses-and-conditions/blood-and-lymph/deep-vein-thrombosis
https://www.healthline.com/health/deep-venous-thrombosis
https://www.webmd.com/dvt/deep-vein-thrombosis-treatment-dvt
https://www.radiologyinfo.org/en/info.cfm?pg=thrombo https://www.ncbi.nlm.nih.gov/books/NBK425364/