Overview
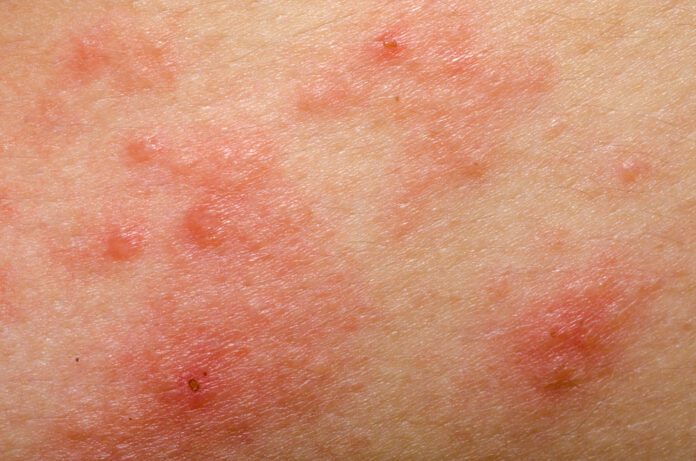
Eczema, also known as atopic dermatitis, is an inflammatory skin condition that causes a scaly, inflamed, itchy rash. It can affect people of all ages, although it occurs more frequently in children (generally before the age of five) than adults.
Although the exact cause of eczema is unknown, it is believed to be the result of both genetic and environmental factors. Since there are no tests available to diagnose eczema, the disease will be confirmed based on a physical exam and whether the symptoms meet specific diagnostic criteria.
Eczema usually starts on the face followed by the hands and feet. Older children tend to be affected in the elbow and knee creases, neck, wrists, ankles, and feet. The hands and feet tend to be the most commonly affected areas in adults. Eczema is not a contagious condition.
Commonly Associated With
Infantile eczema; Dermatitis – atopic; Eczema
Cause
We don’t know what exactly causes eczema. However, for most types of eczema, researchers believe a combination of genes and triggers are involved.
People with eczema tend to have an over-reactive immune system that when triggered by a substance outside or inside the body, responds by producing inflammation. It is this inflammation that causes the red, itchy, and painful skin symptoms common to most types of eczema.
Research also shows that some people with eczema have a mutation of the gene responsible for creating filaggrin. Filaggrin is a protein that helps our bodies maintain a healthy protective barrier on the very top layer of the skin. Without enough filaggrin to build a strong skin barrier, moisture can escape and bacteria, viruses and more can enter. This is why many people with eczema have very dry and infection-prone skin.
Symptoms
● In infants and children, the rash usually occurs on the scalp, knees, elbows, and cheeks.
● In adults, the rash can occur on the creases of wrists, elbows, knees, ankles, face, and neck.
● The rash is usually itchy, red, and scaly. Scratch marks often occur due to the itchy nature of the rash. If one has this rash for a long period of time the affected skin can become thicker.
● Dry skin can worsen the itching and rash. An “itch-scratch cycle” can occur with rubbing or scratching the skin causing more irritation, and thus, additional itching.
● The rash can become worse after eating certain foods. In the case of eczema, this is usually a delayed reaction. However, other reactions to foods can occur more immediately, including hives (itchy welts) and swelling. Allergy testing, either by blood (blood draw) or allergy skin prick (“pricking” foods in a liquid form on the arms or back and waiting 10-15 minutes for an “itchy bump” to occur, indicating an allergy) may be performed by an allergist/immunologist to determine a possible presence of an immediate food allergy. Allergy tests are often positive even in patients who tolerate the food in their diet, and thus foods should not be removed from the diet solely based on the results of these tests.
● Dry skin can worsen the itching and rash. An “itch-scratch cycle” can occur with rubbing or scratching the skin causing more irritation, and thus, additional itching
Eczema is a chronic condition with no known cure. When an eczema flare occurs, the appropriate treatment will vary based on the severity of the rash.
Treatment
Common eczema treatments
OTC PRODUCTS
Over-the-counter (OTC) treatments are products or medications that can be bought without a prescription. Some OTC eczema treatments are used for moisturizing skin; some are used to help skin symptoms such as rash, redness, and itch; and some are for gently cleaning skin to prevent infection.
BATHING
The most effective way to treat dry skin is to give it the moisture it needs through proper bathing and moisturizing. Soak in a warm bath or take a shower and then moisturize immediately afterward (within three minutes). Can also help calm specific symptoms of eczema by adding bleach, vinegar, salt, oatmeal, or baking soda to the bathwater.
MOISTURIZING
When the skin gets too dry, it can become irritated and cause eczema to flare. Wind, low humidity, cold temperatures, harsh soaps, and too much washing without the use of a moisturizer immediately after, all can lead to dry skin.
Many people with eczema have drier-than-normal skin due to an imbalance in the topmost protective layer of skin called the skin barrier. When functioning normally, our skin barrier helps keep irritants and allergens out and moisture in. That’s why bathing and properly moisturizing to maintain a healthy skin barrier are key to help control the eczema symptoms. It’s important to understand how and when to properly moisturize, and which products are best to use when you have eczema.
PRESCRIPTION TOPICALS
Prescription topical medications include corticosteroids (steroids), PDE4 inhibitors, topical calcineurin inhibitors (TCIs), and skin barrier creams. Available through the doctor, these medications are applied to the affected area of the skin to help ease redness, rash, dryness, and itching.
PHOTOTHERAPY
In phototherapy, a special machine is used to emit narrowband ultraviolet B (UVB) light onto the skin to help reduce itching and inflammation, increase vitamin D production and bacteria-fighting systems in the skin.
SYSTEMIC MEDICATIONS (IMMUNOSUPPRESSANTS)
While the exact cause of eczema is not known, researchers understand that that the immune system is involved. In eczema, the immune system overreacts and produces inflammation, which leads to symptoms such as itching, redness, and skin barrier problems.
If you have severe eczema, The doctor may prescribe a type of medication called an immunosuppressant. An immunosuppressant drug helps control, or suppress, the immune system to slow down the symptoms of severe eczema.
BIOLOGICS
Biologic drugs or “biologics” target a particular piece of the immune system reaction that contributes to atopic dermatitis symptoms. They contain genetically engineered proteins derived from human genes and are administered intravenously (through the vein) as infusions to target specific parts of the immune system that trigger inflammation.
COMPLEMENTARY AND ALTERNATIVE THERAPIES
Studies have shown that certain complementary and alternative therapies can be beneficial in controlling the symptoms of eczema. These include some supplements, plant-based topicals such as coconut oils, meditation, and biofeedback.
Other
Eczema triggers
Working to keep your symptoms under control is important to staying healthy and comfortable while living with eczema. When trying to identify potential triggers, keep in mind that an eczema flare can appear sometime after exposure. This lag time can make some triggers challenging to detect.
Eczema affects everyone differently. One person’s triggers may not be the same as another’s. You might experience eczema symptoms at certain times of the year or in different areas of your body.
Common triggers include:
• Dry skin. When your skin gets too dry, it can easily become brittle, scaly, rough, or tight, which can lead to an eczema flare-up.
Learn more about the importance of moisturizing skin to manage eczema flares.
• Irritants. Everyday products and even natural substances can cause your skin to burn and itch, or become dry and red. These can include products that you use on your body or in your home — hand and dish soap, laundry detergent, shampoo, bubble bath, and body wash, or surface cleaners and disinfectants. Even some natural liquids, like the juice from fresh fruit, vegetables, or meats, can irritate your skin when you touch them.
Common irritants include:
- metals (especially nickel)
- cigarette smoke
- soaps and household cleansers
- fragrances
- certain fabrics like wool and polyester
- antibacterial ointments like neomycin and bacitracin
- formaldehyde, which is found in household disinfectants, some vaccines, glues, and adhesives
- isothiazolinone, an antibacterial that is found in personal care products like baby wipes
- cocamidopropyl betaine, which is used to thicken shampoos and lotions
- paraphenylene-diamine, which is used in leather dyes and temporary tattoos, among others
Source
https://www.verywellhealth.com/eczema-overview-4688797
https://www.southerncross.co.nz/group/medical-library/eczema-causes-symptoms-treatment
https://nationaleczema.org/eczema/treatment/
https://www.verywellhealth.com/eczema-overview-4688797
https://www.aaaai.org/conditions-and-treatments/library/allergy-library/eczema-atopic-dermatitis