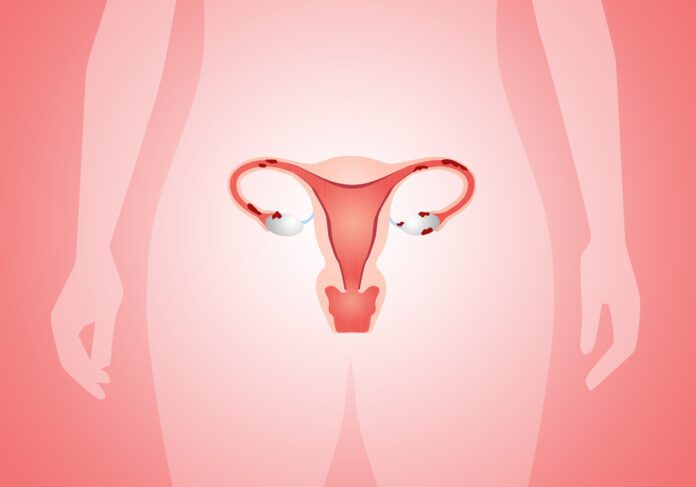
Overview
Endometriosis is a disorder in which tissue similar to the tissue that forms the lining of the uterus grows outside of the uterine cavity. The lining of the uterus is called the endometrium.
Endometriosis occurs when endometrial tissue grows on the ovaries, bowel, and tissues lining the pelvis. It’s unusual for endometrial tissue to spread beyond the pelvic region, but it’s not impossible. Endometrial tissue growing outside of the uterus is known as an endometrial implant.
The hormonal changes of the menstrual cycle affect the misplaced endometrial tissue, causing the area to become inflamed and painful. This means the tissue will grow, thicken, and break down. Over time, the tissue that has broken down has nowhere to go and becomes trapped in the pelvis.
This tissue trapped in the pelvis can cause:
● irritation
● scar formation
● adhesions, in which tissue binds the pelvic organs together
● severe pain during the periods
● fertility problems
Endometriosis is a common gynecological condition.
Cause
The cause of endometriosis is unknown.
Who is at risk for endometriosis?
Endometriosis is most commonly diagnosed in women in their 30s and 40s. But it can affect any female who menstruates. Certain factors can raise or lower your risk of getting it.
You are at higher risk if
• You have a mother, sister, or daughter with endometriosis
• Your period started before age 11
• Your monthly cycles are short (less than 27 days)
• Your menstrual cycles are heavy and last more than 7 days
You have a lower risk if
• You have been pregnant before
• Your periods started late in adolescence
• You regularly exercise more than 4 hours a week
• You have a low amount of body fat
Symptoms
The symptoms of endometriosis vary. Some women experience mild symptoms, but others can have moderate to severe symptoms. The severity of the pain doesn’t indicate the degree or stage of the condition. You may have a mild form of the disease yet experience agonizing pain. It’s also possible to have a severe form and have very little discomfort.
Pelvic pain is the most common symptom of endometriosis. You may also have the following symptoms:
● painful periods
● pain in the lower abdomen before and during menstruation
● cramps one or two weeks around menstruation
● heavy menstrual bleeding or bleeding between periods
● pain following sexual intercourse
● discomfort with bowel movements
● lower back pain that may occur at any time during the menstrual cycle
At times there are no symptoms.
Treatment
There’s no cure for endometriosis and it can be difficult to treat. Treatment aims to ease symptoms so the condition does not interfere with daily life.
Treatment options available to women with endometriosis are:
● Surgery
Doctors perform two main types of surgery to treat endometriosis:
Conservative surgery removes as much of the endometrial tissue as possible but preserves the reproductive organs (ovaries and uterus). When the doctor does this procedure through small incisions, it’s called laparoscopy. Laparoscopy can also be used to diagnose endometriosis.
Hysterectomy treats more severe endometriosis. The surgeon removes the uterus, and possibly the cervix and ovaries. If you have this surgery, you’ll no longer be able to get pregnant.
● Hormone treatment
As endometriosis responds and grows when exposed to the female hormone oestrogen, several hormone treatments attempt to block or reduce the production of oestrogen in the body. This means the endometriosis will be unable to continue growing and will help to relieve symptoms.
● Pain relief
Heat and comfort – A simple hot water bottle or a hot bath may help to reduce pain. Some women also find heated wheat bags to be effective. Being comfortable and reducing stress will also be beneficial.
Painkillers – Non-steroidal anti-inflammatory drugs (NSAIDs) such as Ibuprofen, Voltarol, and Ponstan (mefanemic acid) block the production of prostaglandins in the body. Prostaglandins occur naturally, in response to injury or disease, and cause pain and inflammation. They have a number of functions including making the womb contract during a period (which helps with the shedding of the womb lining). These contractions can cause pain. It is thought that women with endometriosis may produce more prostaglandins than women without the condition.
Physiotherapy – Physiotherapists can develop a program of exercise and relaxation techniques designed to help strengthen pelvic floor muscles, reduce pain, and manage stress and anxiety. After surgery, rehabilitation in the form of gentle exercises, yoga, or Pilates can help the body get back into shape by strengthening compromised abdominal and back muscles.
Pain modifiers – These drugs work by altering the body’s perception of pain.
Pain clinics – Some hospitals and trusts have specialized pain clinics providing advice and support to people in chronic pain.
Transcutaneous Electrical Nerve Stimulator (TENS) machines – TENS machines are an alternative to painkillers. They are small, unobtrusive machines with electrodes that attach to the skin and send electrical pulses into the body. This does not hurt but instead feels mildly ticklish. The electrical pulses are thought to work by either blocking the pain messages as they travel through the nerves or by helping the body produce endorphins which are natural pain-fighters. Some TENS machines can be clipped to a belt.
Other
How is endometriosis diagnosed?
Surgery is the only way to know for sure that you have endometriosis. First, however, your health care provider will ask about your symptoms and medical history. You will have a pelvic exam and may have some imaging tests.
The surgery to diagnose endometriosis is a laparoscopy. This is a type of surgery that uses a laparoscope, a thin tube with a camera and light. The surgeon inserts the laparoscope through a small cut in the skin. Your provider can make a diagnosis based on how the patches of endometriosis look. He or she may also do a biopsy to get a tissue sample.
Source
https://www.healthline.com/health/endometriosis
https://www.nhs.uk/conditions/endometriosis/treatment/
https://www.endometriosis-uk.org/pain-relief-endometriosis#TENS